Real-Time Eligibility & Claims StatusBuilt for Scale
Instant, accurate eligibility verification and claims status checks across 3,500+ payers nationally. Single or batch processing. No manual lookups. No delays.
3,500+
Payers Covered
98%
Clean Claim Rate
<20s
Avg. Response Time
24/7
Availability
Core Capabilities
Two Services. One Platform. Zero Delays.
WeRrcm specializes in real-time eligibility verification and claims status checks -- available as single or batch, covering 3,500+ payers nationally.
Payers Covered Nationally
Comprehensive coverage across all major commercial, Medicare, and Medicaid payers
Real-Time Eligibility Verification
270/271 Transactions
Instantly verify patient insurance coverage, benefits, and eligibility before the point of service. Prevent denials at the front door with accurate, real-time data from 3,500+ payers.
- Real-time 270/271 transaction processing
- Patient demographics and coverage validation
- Co-pay, deductible, and out-of-pocket details
- Prior authorization requirements check
- Active/inactive coverage status verification
- Multi-payer batch processing support
Real-Time Claims Status & Acknowledgement
276/277 Transactions
Track claim status from submission through adjudication in real time. Get instant acknowledgments, identify rejections early, and accelerate your revenue cycle.
- Real-time 276/277 status inquiries
- Claim acknowledgment (TA1/999) tracking
- Adjudication status and payment details
- Rejection and denial reason code mapping
- Automated follow-up on pending claims
- Batch status checks across all payers
Instant Results
<2 second response time
Zero Manual Lookups
Fully automated verification
HIPAA Compliant
SOC 2 certified platform
Coverage Across All Major Payers
Real-time eligibility verification for 3,500+ commercial, Medicare, and Medicaid payers
Why WeRrcm
Intelligent Automation for Every Step of Your Revenue Cycle
Our end-to-end platform eliminates bottlenecks, reduces manual work, and maximizes reimbursement across your entire healthcare organization.
AI-Powered Coding
Leverage advanced AI to automate medical coding with unprecedented accuracy. Our system continuously learns from patterns to improve claim acceptance rates.
Automated Claim Submission
Eliminate manual errors with intelligent claim scrubbing and automated electronic submission to all major payers within hours, not days.
Denial Management
Proactively identify and resolve denials with AI-driven root cause analysis. Automatically appeal and rework claims to recover maximum revenue.
Real-Time Analytics
Gain actionable insights with comprehensive dashboards tracking KPIs across your revenue cycle. Make data-driven decisions in real time.
AI-Powered HIPAA Compliance
Built from the ground up with AI-driven security and compliance. Real-time PHI monitoring, automated breach prevention, and immutable audit trails protect every transaction.
Faster Reimbursement
Accelerate cash flow with streamlined workflows that cut days in A/R by up to 40%. Get paid faster with fewer touchpoints.
Monthly Recovery
+$1.2M
Avg. per client / month
End-to-End Services
Complete Revenue Cycle Coverage
From the first patient touchpoint through final reimbursement, WeRrcm covers every phase of your revenue cycle.
Patient Registration & Eligibility
Automated insurance verification, eligibility checks, and prior authorization at the point of scheduling to prevent front-end denials.
Charge Capture & Coding
AI-assisted charge capture and ICD-10/CPT coding ensures maximum accuracy and compliance across all specialties and payer requirements.
Claims Submission & Tracking
Electronic claim submission with built-in scrubbing, real-time status tracking, and automated follow-up to ensure timely processing.
Payment Posting & Reconciliation
Automated ERA/EOB posting, payment reconciliation, and patient statement generation with transparent balance reporting.
Denial Prevention & Appeals
Predictive denial analytics, automated appeal generation, and root cause tracking to systematically reduce denial rates.
Reporting & Business Intelligence
Executive dashboards, payer performance analytics, and actionable insights to optimize financial performance across your organization.
Complete RCM Lifecycle
End-to-End Revenue Cycle Automation
WeRrcm automates every stage of the Revenue Cycle Management lifecycle -- from patient scheduling through final collections -- connecting Providers, Patients, and Payers in one intelligent platform.
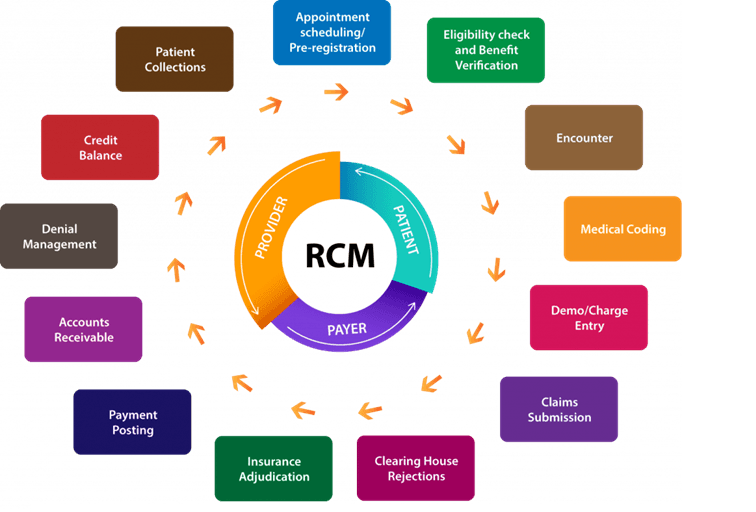
How WeRrcm Automates Every Step
Appointment Scheduling / Pre-registration
Automated patient scheduling with real-time pre-registration data capture and demographic verification.
Eligibility Check & Benefit Verification
AI-driven real-time insurance eligibility verification and benefit coverage analysis before the patient visit.
Encounter
Seamless clinical encounter documentation integration ensuring complete and accurate charge capture.
Medical Coding
AI-assisted CPT, ICD-10, and HCPCS coding with compliance validation and accuracy checks.
Demo / Charge Entry
Automated demographic and charge entry with intelligent field mapping and error prevention.
Claims Submission
Clean claim submission with automated scrubbing, payer-specific formatting, and electronic filing.
Clearing House Rejections
Instant rejection identification with automated correction workflows and re-submission tracking.
Insurance Adjudication
End-to-end payer adjudication tracking with automated follow-up and appeal management.
Payment Posting
Automated ERA/EOB processing, payment matching, and variance identification for fast reconciliation.
Accounts Receivable
Intelligent A/R management with aging analysis, prioritized worklists, and automated follow-up.
Denial Management
AI-powered denial root cause analysis, automated appeals, and prevention strategies to reduce future denials.
Credit Balance
Automated credit balance identification, resolution workflows, and refund processing to ensure compliance.
Patient Collections
Patient-friendly billing with automated statements, payment plans, and digital payment options.
13
Lifecycle Steps
3
Stakeholders Connected
100%
Automated Workflow
1
Unified Platform
Our Process
How WeRrcm Transforms Your Revenue Cycle
A seamless, automated workflow from patient intake to final reimbursement. Click any step to see how we automate it.
Automated eligibility checks and prior authorizations verify coverage before services are rendered, preventing costly denials upfront.
AI-driven medical coding ensures ICD-10 and CPT accuracy. Charges are captured in real time and validated against payer-specific rules.
Multi-layer claim scrubbing catches errors before submission. Claims are electronically filed to clearinghouses and payers with full tracking.
Automated payment posting, denial identification, and intelligent appeal workflows ensure maximum reimbursement with minimal manual effort.
Comprehensive analytics dashboards deliver actionable insights, enabling continuous improvement and strategic financial decision-making.
Results That Matter
Measurable Impact on Your Revenue Cycle
Real numbers. Real results. Built for medical billing teams and RCM professionals who demand accuracy and speed.
3,500+
Payers Covered Nationally
Comprehensive payer coverage across commercial, Medicare, and Medicaid
98%
First-Pass Clean Claim Rate
Industry-leading accuracy through real-time claim scrubbing
40%
Reduction in Denials
Proactive denial prevention with automated root cause analysis
<20s
Avg. Response Time
Instant eligibility and claims status results in under 20 seconds
HIPAA Compliance, Automated by AI
WeRrcm integrates AI at every layer of HIPAA compliance. From real-time PHI monitoring to automated breach prevention, our platform ensures your organization meets and exceeds all federal regulatory requirements.
100%
HIPAA Audit Pass Rate
0
Data Breaches Since Inception
<1s
Threat Detection Response
24/7
Compliance Monitoring
AI-Driven Risk Detection
Our intelligent models continuously scan every transaction, flagging potential HIPAA violations before they occur. Automated risk scoring prioritizes issues for immediate remediation.
End-to-End Encryption
All patient data is encrypted in transit and at rest using AES-256 encryption. Zero-trust architecture ensures no unauthorized access at any point in the revenue cycle.
Real-Time PHI Monitoring
AI-powered surveillance tracks every access to Protected Health Information. Instant alerts notify compliance officers of suspicious activity 24/7.
Automated Audit Trails
Every action is logged with immutable, tamper-proof audit trails. AI generates comprehensive compliance reports on demand for OCR audits and internal reviews.
Secure Cloud Infrastructure
HIPAA-compliant cloud hosting with BAA agreements, automated backups, disaster recovery, and geo-redundant data centers across the United States.
Breach Prevention Engine
Machine learning algorithms analyze access patterns to detect anomalies. Automated containment protocols activate instantly to prevent data breaches.
Our HIPAA Compliance Guarantee
Every WeRrcm deployment undergoes rigorous HIPAA validation. Our AI continuously monitors administrative, physical, and technical safeguards to ensure your organization remains compliant at all times.
Proven Impact
Measurable Results from Real Implementations
Data-driven outcomes from healthcare organizations using WeRrcm for real-time eligibility and claims processing.
Pilot Program Results
38%
Average reduction in front-end denials
96%+
First-pass clean claim rate achieved
<30s
Average eligibility response time
$500K+
Average monthly revenue recovered per client
450-bed Hospital Network
"Reduced front-end denials by 35% in the first quarter after switching to WeRrcm's real-time eligibility verification."
— Chief Medical Officer
Multi-Specialty Billing Company
"First-pass clean claim rate improved from 78% to 96% within 60 days. Recaptured $800K in previously lost revenue."
— VP of Revenue Cycle
15-Provider Physician Group
"Eliminated 4 hours of daily manual eligibility checks. Staff now focuses on patient care instead of payer portals."
— Director of Finance
Results based on WeRrcm pilot implementations. Individual results may vary.
Our Leadership
Driven by Purpose, Powered by Innovation
WeRrcm was founded with a clear mission: to eliminate the inefficiencies plaguing healthcare revenue cycles across America. Under the leadership of CEO Manikandan Govindan, our team combines deep healthcare domain expertise with cutting-edge technology to deliver measurable results.

Manikandan Govindan
Chief Executive Officer
A visionary leader with over 20 years of experience in healthcare technology and revenue cycle operations, Manikandan drives WeRrcm's mission to transform healthcare financial management through intelligent automation.
Our Mission
To empower healthcare providers with intelligent automation that maximizes revenue, minimizes administrative burden, and lets clinicians focus on what matters most - patient care.
Our Vision
A healthcare ecosystem where every provider, regardless of size, has access to world-class revenue cycle technology that ensures financial sustainability.
Our Values
Integrity, innovation, and impact guide everything we do. We measure our success by the measurable outcomes we deliver to our clients and their patients.
Contact Us
Ready to Transform Your Revenue Cycle?
Schedule a personalized demo and discover how WeRrcm can automate your end-to-end RCM process, reduce denials, and maximize revenue.
Get in Touch
Reach out to our team directly. We respond within 24 hours.
Why Choose WeRrcm?
- 98% Clean Claim Rate
- 30% Reduction in Denials
- End-to-End Automation
- HIPAA Compliant & SOC 2 Certified
- Dedicated Account Manager
Schedule a Demo
Fill out the form below and our team will get back to you within 24 hours.
Try WeRrcm Free — No Commitment Required
500 eligibility verifications free. See your denial reduction in 30 days. Cancel anytime.